Endometrial cancer is the most common type of uterine cancer. Find out what causes it, how to spot the warning signs, and what treatments are available.
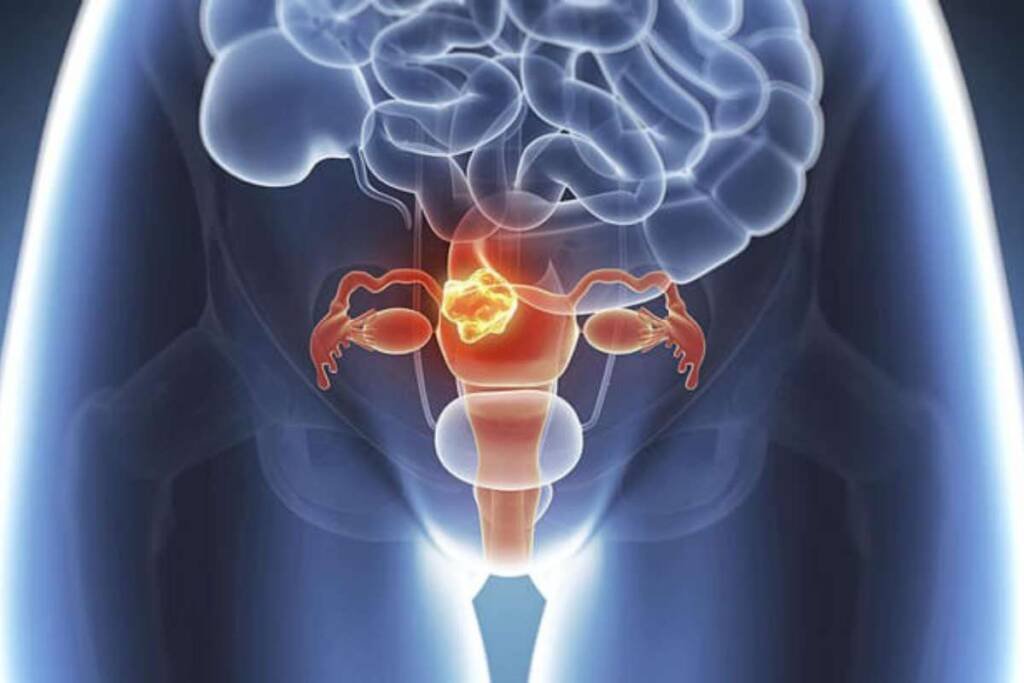
Endometrial cancer is a type of cancer that affects the lining of the uterus, the organ where a baby grows during pregnancy. It is one of the most common cancers in women, especially after menopause. But don’t panic! Endometrial cancer can be detected early and treated effectively, if you know the signs and symptoms, the causes and risk factors, and the available treatment options. In this blog post, we will give you an overview of endometrial cancer and answer some frequently asked questions.
Endometrial Cancer: An Introduction
Endometrial cancer is a cancer that starts in the endometrium, the inner layer of cells that form the lining of the uterus. The endometrium changes throughout the menstrual cycle, thickening to prepare for a possible pregnancy and shedding during menstruation. Sometimes, abnormal cells can grow in the endometrium and form a tumor. These cells can invade deeper into the uterine wall or spread to other parts of the body.
Endometrial cancer is sometimes called uterine cancer, but this term can also refer to other types of cancer that occur in the uterus, such as uterine sarcoma, which is much less common. Endometrial cancer is more likely to occur in women who have gone through menopause, but it can also affect younger women.
According to the American Cancer Society, about 66,570 new cases of endometrial cancer will be diagnosed in 2021, and about 12,940 women will die from it. The average age at diagnosis is 60 years old. The five-year survival rate for endometrial cancer is 81%, but it varies depending on the stage and type of the cancer.

What are the symptoms of endometrial cancer?
The most common symptom of endometrial cancer is abnormal vaginal bleeding. This may include:
- Bleeding after menopause
- Bleeding between periods
- Heavier or longer periods than usual
- Spotting or discharge that is pink, red, or brown
- Other symptoms of endometrial cancer may include:
- Pelvic pain or pressure
- Difficulty or pain when urinating
- Pain during sex
- Unexplained weight loss
These symptoms are not specific to endometrial cancer and may be caused by other conditions. However, if you have any of these symptoms, especially abnormal bleeding, you should see your doctor as soon as possible.
What are the causes of endometrial cancer?
The exact cause of endometrial cancer is not known, but it is thought to be related to changes in the balance of female hormones in the body. Hormones are chemical messengers that regulate various functions in the body. The main female hormones are estrogen and progesterone, which affect the growth and shedding of the endometrium.
Normally, estrogen and progesterone work together to keep the endometrium healthy. Estrogen causes the endometrium to thicken during the first half of the menstrual cycle, while progesterone prepares it for a possible pregnancy during the second half. If no pregnancy occurs, both hormones drop and the endometrium is shed during menstruation.
However, sometimes there may be too much estrogen and not enough progesterone in the body. This can cause the endometrium to grow too much and become abnormal. Over time, these abnormal cells may turn into cancer.
What are the risk factors of endometrial cancer?
A risk factor is anything that increases your chance of getting a disease. Having a risk factor does not mean that you will get endometrial cancer, and not having a risk factor does not mean that you will not get it. However, knowing your risk factors can help you make informed decisions about your health.
Some of the risk factors for endometrial cancer are:
- Age: The risk of endometrial cancer increases with age, especially after menopause.
- Obesity: Being overweight or obese increases the amount of estrogen in your body, which can stimulate the growth of the endometrium.
- Hormone therapy: Taking estrogen alone after menopause (without progesterone) can increase your risk of endometrial cancer. However, taking estrogen with progesterone (combined hormone therapy) may lower your risk.
- Tamoxifen: This is a drug used to treat breast cancer or prevent it from coming back. It acts like estrogen on some tissues in your body, such as the endometrium.
- Family history: Having a close relative (such as a mother or sister) who had endometrial cancer may increase your risk.
- Genetic syndromes: Some inherited conditions can increase your risk of endometrial cancer, such as Lynch syndrome or Cowden syndrome.
Other medical conditions: Having diabetes, high blood pressure, polycystic ovary syndrome, or endometrial hyperplasia (a benign condition where the endometrium is thicker than normal) can increase your risk of endometrial cancer.
Also Read: Trodelvy: The New Hope For Breast Cancer Patients
How is endometrial cancer diagnosed?
If you have symptoms of endometrial cancer, your doctor will ask you about your medical history, perform a physical exam, and order some tests to confirm the diagnosis. Some of the tests that may be used are:
- Pelvic exam: Your doctor will examine your vulva, vagina, cervix, uterus, ovaries, and rectum for any abnormalities.
- Transvaginal ultrasound: Your doctor will insert a wand-like device into your vagina that uses sound waves to create images of your uterus. This can show the thickness and texture of your endometrium and help rule out other conditions.
- Hysteroscopy: Your doctor will insert a thin, flexible tube with a light and a camera into your uterus through your vagina and cervix. This allows your doctor to see the inside of your uterus and the endometrium.
- Endometrial biopsy: Your doctor will remove a small sample of tissue from your endometrium using a thin tube or a suction device. The tissue will be sent to a lab for analysis under a microscope to look for cancer cells.
- Dilation and curettage (D&C): Your doctor will dilate (widen) your cervix and scrape or suction tissue from your endometrium. This can provide more tissue for analysis than a biopsy. This procedure is usually done under anesthesia in an operating room.
If endometrial cancer is found, your doctor will refer you to a specialist who treats cancers of the female reproductive system (gynecologic oncologist). The specialist will perform more tests to determine the stage and type of your cancer. The stage indicates how far the cancer has spread in your body, while the type indicates how the cancer cells look under a microscope. The stage and type of your cancer will affect your treatment options and prognosis.

What are the treatment options for endometrial cancer?
The main treatment options for endometrial cancer are surgery, radiation therapy, chemotherapy, and targeted therapy. The best treatment for you will depend on several factors, such as the stage and type of your cancer, your age and overall health, your preferences and goals, and the potential benefits and side effects of each option. Your treatment plan may include one or more of the following:
Surgery in endometrial cancer
Surgery is the most common treatment for endometrial cancer. The goal of surgery is to remove as much of the cancer as possible and to find out if it has spread to nearby lymph nodes or other organs. The main type of surgery for endometrial cancer is hysterectomy, which is the removal of the uterus. Depending on the extent of the cancer, you may also need to have one or both ovaries and fallopian tubes removed (salpingo-oophorectomy), some lymph nodes in the pelvis or abdomen removed (lymph node dissection), or other organs that are affected by the cancer removed (debulking surgery).
Surgery can be done through an incision in your abdomen (open surgery) or through several small incisions using a thin tube with a light and a camera (laparoscopic surgery). Laparoscopic surgery may also involve the use of a robotic device that allows more precise movements (robotic surgery). Laparoscopic surgery usually has less blood loss, pain, infection, and scarring than open surgery. However, not all women are candidates for laparoscopic surgery.
Surgery can cure early-stage endometrial cancer in most cases. However, it also has some risks and side effects, such as bleeding, infection, injury to nearby organs, blood clots, nerve damage, urinary problems, bowel problems, sexual dysfunction, menopause symptoms (if you have your ovaries removed), and infertility (if you have your uterus removed).
Radiation therapy in endometrial cancer
Radiation therapy uses high-energy rays or particles to kill cancer cells or stop them from growing. Radiation therapy can be given before surgery to shrink the tumor or after surgery to destroy any remaining cancer cells. Radiation therapy can also be used as the main treatment for women who cannot have surgery or as a palliative treatment for women with advanced or recurrent endometrial cancer.
Radiation therapy can be given in two ways:
External beam radiation therapy: A machine outside your body delivers radiation to a specific area where the cancer is located. You may receive several treatments over several weeks.
Internal radiation therapy (brachytherapy): A device containing radioactive material is placed inside your vagina or uterus for a short time. You may receive one or more treatments over several days.
Radiation therapy can help control endometrial cancer and prevent it from coming back. However, it also has some side effects, such as skin irritation, fatigue, nausea, diarrhea, bladder problems, vaginal dryness or narrowing, sexual dysfunction, menopause symptoms (if you have your ovaries exposed to radiation), and infertility (if you have your uterus exposed to radiation).
Chemotherapy in endometrial cancer
Chemotherapy uses drugs to kill cancer cells or stop them from growing. Chemotherapy can be given before surgery to shrink the tumor or after surgery to destroy any remaining cancer cells. Chemotherapy can also be used as the main treatment for women with advanced or recurrent endometrial cancer that has spread to other parts of the body.
Chemotherapy can be given in different ways:
Intravenous (IV) chemotherapy: The drugs are injected into a vein, usually in your arm or chest. You may receive several treatments over several weeks or months.
Oral chemotherapy: The drugs are taken as pills or capsules by mouth. You may take them at home or at a clinic.
Intraperitoneal (IP) chemotherapy: The drugs are injected into the abdominal cavity, where they can reach the cancer cells more directly. You may receive this treatment in a hospital or a clinic.
Chemotherapy can help control endometrial cancer and improve survival. However, it also has some side effects, such as hair loss, mouth sores, loss of appetite, nausea, vomiting, diarrhea, fatigue, infection, bleeding, nerve damage, kidney problems, liver problems, heart problems, sexual dysfunction, menopause symptoms (if you have your ovaries affected by chemotherapy), and infertility (if you have your uterus affected by chemotherapy).
Targeted therapy in endometrial cancer
Targeted therapy uses drugs that target specific molecules or genes that are involved in the growth and spread of cancer cells. Targeted therapy can be given alone or in combination with other treatments for endometrial cancer. Targeted therapy can also be used as a palliative treatment for women with advanced or recurrent endometrial cancer that does not respond to other treatments.
Targeted therapy can be given in different ways:
Intravenous (IV) targeted therapy: The drugs are injected into a vein, usually in your arm or chest. You may receive several treatments over several weeks or months.
Oral targeted therapy: The drugs are taken as pills or capsules by mouth. You may take them at home or at a clinic.
Some of the targeted drugs that are approved or being tested for endometrial cancer are:
- Lenvatinib (Lenvima): This drug blocks the action of several proteins that stimulate the growth of blood vessels that feed the tumor. It is approved in combination with pembrolizumab (Keytruda), an immunotherapy drug that boosts the immune system’s ability to fight cancer cells, for women with advanced endometrial cancer that is not MSI-H or dMMR.
- Pembrolizumab (Keytruda): This drug blocks the action of a protein called PD-1 that prevents the immune system from attacking cancer cells. It is approved alone or in combination with lenvatinib for women with advanced endometrial cancer that is MSI-H or dMMR.
- Dostarlimab (Jemperli): This drug blocks the action of a protein called PD-L1 that prevents the immune system from attacking cancer cells. It is approved for women with advanced endometrial cancer that is MSI-H or dMMR and has progressed after prior treatment.
- Olaparib (Lynparza): This drug blocks the action of an enzyme called PARP that helps repair DNA damage in cancer cells. It is being tested in combination with cediranib (Recentin), a drug that blocks the action of a protein called VEGF that stimulates the growth of blood vessels that feed the tumor, for women with recurrent endometrial cancer.
Targeted therapy can help control endometrial cancer and delay its progression. However, it also has some side effects, such as rash, diarrhea, high blood pressure, fatigue, nausea, vomiting, liver problems, kidney problems, lung problems, heart problems, and blood clots.
What are the emerging treatment options for endometrial cancer?
Endometrial cancer research is ongoing and new treatment options are being developed and tested. Some of the emerging treatment options for endometrial cancer are:
- Immunotherapy: This is a type of treatment that uses substances made by the body or in a lab to boost the immune system’s ability to fight cancer cells. Besides pembrolizumab and dostarlimab, other immunotherapy drugs that are being tested for endometrial cancer include atezolizumab (Tecentriq), nivolumab (Opdivo), ipilimumab (Yervoy), and durvalumab (Imfinzi).
- Hormone therapy: This is a type of treatment that uses drugs that block the production or action of hormones that stimulate the growth of hormone-sensitive cancers. Some hormone therapy drugs that are being tested for endometrial cancer include letrozole (Femara), anastrozole (Arimidex), exemestane (Aromasin), and megestrol acetate (Megace).
- CAR T-cell therapy: This is a type of treatment that uses genetically modified immune cells (T cells) that are programmed to recognize and kill cancer cells. Some CAR T-cell therapies that are being tested for endometrial cancer target proteins such as MUC16, HER2, or mesothelin.
- Vaccine therapy: This is a type of treatment that uses substances that stimulate the immune system to recognize and attack cancer cells. Some vaccine therapies that are being tested for endometrial cancer use peptides, viruses, or bacteria that carry antigens or genes related to the cancer.
Also Read: How To Deal With Enlarged Prostate In Young Males: Symptoms, Causes And Treatment Options
Future directions of endometrial cancer
Endometrial cancer is a complex and heterogeneous disease that requires personalized and multidisciplinary care. The future directions of endometrial cancer include:
- Improving the prevention and early detection of endometrial cancer by identifying and modifying risk factors, developing and implementing screening tests, and promoting awareness and education.
- Improving the diagnosis and staging of endometrial cancer by using molecular and genetic tests, imaging techniques, and biomarkers to classify the cancer into subtypes and predict its behavior and response to treatment.
- Improving the treatment and survival of endometrial cancer by developing and testing new drugs, combinations, and modalities, as well as optimizing the existing ones, based on the characteristics and preferences of each patient.
- Improving the quality of life and well-being of endometrial cancer survivors by addressing the physical, emotional, social, and financial challenges they face after treatment, as well as providing them with supportive care and follow-up services.
Conclusion
Endometrial cancer is a common and treatable type of cancer that affects the lining of the uterus. It can cause abnormal vaginal bleeding and other symptoms. It is caused by changes in the balance of female hormones in the body. It can be diagnosed by various tests, such as pelvic exam, ultrasound, biopsy, or D&C. It can be treated by various options, such as surgery, radiation therapy, chemotherapy, or targeted therapy. It can also be prevented or detected early by modifying risk factors, undergoing screening tests, or seeking medical attention promptly.
Endometrial cancer research is advancing rapidly and new treatment options are emerging. The future of endometrial cancer is promising and hopeful. If you have endometrial cancer or know someone who does, you are not alone. There are many resources and support groups available to help you cope with this disease. You can also participate in clinical trials or donate to research organizations to contribute to the fight against endometrial cancer.
FAQ’s
How common is endometrial cancer?
Endometrial cancer is the most common type of gynecologic cancer in the United States. It accounts for about 3% of all cancers in women. It is estimated that 1 in 37 women will develop endometrial cancer in their lifetime.
What is the difference between endometrial cancer and uterine sarcoma?
Endometrial cancer starts in the endometrium, the inner lining of the uterus. Uterine sarcoma starts in the muscle layer (myometrium) or connective tissue (stroma) of the uterus. Uterine sarcoma is much rarer than endometrial cancer. It accounts for about 2% to 4% of all uterine cancers. It is also more aggressive and harder to treat than endometrial cancer.
What does MSI-H or dMMR mean?
MSI-H stands for microsatellite instability-high. dMMR stands for deficient mismatch repair. These are terms that describe how some cells have defects in their DNA repair mechanisms, which leads to accumulation of mutations in their genes. About 25% to 30% of endometrial cancers have MSI-H or dMMR status. These cancers tend to be more responsive to immunotherapy drugs than other cancers.
Can I get pregnant after having endometrial cancer?
If you have your uterus removed (hysterectomy) as part of your treatment for endometrial cancer, you will not be able to get pregnant naturally. However, you may still have options to have a child using assisted reproductive technologies (ART), such as in vitro fertilization (IVF) with a gestational carrier (surrogate).